Note: I wrote this on August 29, 2020, but never made it public, because I never finished it. However, it is now April 2022, and I am still hearing this same crazy argument, so here is the incomplete version. Since February 2020, there have been one million more deaths in the U.S. than would be expected. Because expected deaths are very consistent from year to year, something has killed an extra one million people. You can decide for yourself what it might be, but I’m putting my money on COVID-19.
As the death toll from COVID-19 rises, I keep hearing from people that the count is exaggerated because places were essentially counting all deaths as caused by COVID-19. There appears to be some anecdotal evidence for this, but mostly just hospital staff claiming this was happening. I’ve not seen any proof of this, although I’m sure it’s likely happened. I am also certain that the increase in deaths attributed to pneumonia just before the disease was known to be spreading was mostly due to COVID-19. Thus, there has likely been some over- and under-counting.
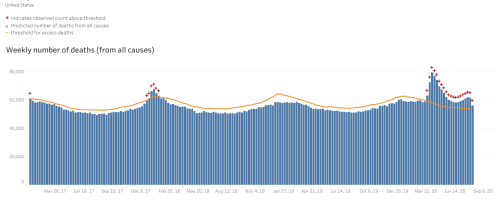
The thing that really cannot be faked is the total number of deaths this year. The number of people dying in a year is fairly consistent and the CDC tracks this. The number of people dying from common causes is also fairly consistent. The CDC tracks what it calls “excess deaths” that try to better understand if there’s an epidemic or pandemic. They have a great web page that allows you to explore this data (CDC Excess Deaths). The data is updated weekly but, as noted on the web page, the most recent few weeks are likely not accurate as death certificates have not been submitted and/or entered into the database. As of August 20, 2020, the graph of all deaths in the US is shown below.
The yellow/orange line in this chart is what the CDC calls the “excess death threshold.”
This line gives a limit beyond which the number of extra deaths for a week could possibly be due to normal variations. This is based on data from 2013 to the current date. The average (from 2013) is not shown on this chart but is available in the data on the page. If deaths for a week exceed this threshold we can be very certain that something is killing people besides the usual causes. You can see the 2017-2018 flu season was particularly bad for about a month but the 2018-2019 season was not nearly as bad. Note, that it is usually excess pneumonia deaths that contribute to excess deaths during flu season. The 2019-2020 flu season also was quite mild and well within what we would expect to see.
As an example of the data shown in this chart, let’s look at the week of June 14, 2020, which is the low point of the excess deaths since the pandemic started. During this week, the threshold for excess deaths was about 54,600 deaths. The average since 2013 for this week is about 52,700. The number of deaths recorded was about 58,300, or 3,700 above the epidemic/pandemic threshold and 5,600 above the average.
For the weeks before the pandemic hit, January 5th through March 8th, the country had slightly fewer deaths (2,500) than average, i.e. the flu season was not particularly bad. However, from March 8th until August 2nd, there have been 214,800 more deaths than normal for that date range and 174,100 more than the epidemic/pandemic threshold. Thus, it is very clear that something is causing many more people to die than would be expected. This also makes it clear that the death toll from COVID-19, which at the time was about 160,000, is probably too low.
You might attribute some of the extra 50,000 deaths (between those attributed to COVID-10 and those over the average) to an increase in suicides. However, the number of suicides in that period would have had to more than double–about 4,000 people kill themselves each month. Plus, the number of deaths from workplace and vehicle accidents have been reported to be significantly down–about 9,000 people die in accidents each month. My best guess is that the increase in suicides is probably offset by the decreases in accidental deaths and COVID-19 has at least contributed to the majority of those 50,000 extra deaths.
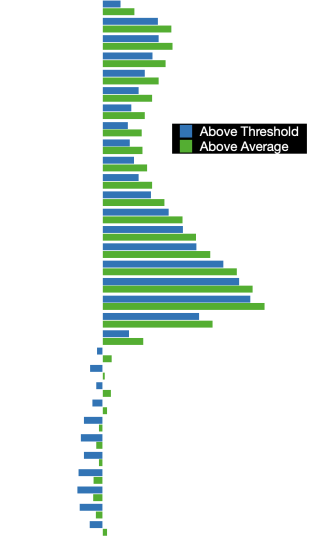
We can chart the number of deaths each week compared to both the average and the epidemic/pandemic threshold.
The chart clearly shows the large number–over 10,000 in most weeks–of deaths above both the average and the threshold from the end of March until the beginning of May. The excess deaths then decreased to a minimum around the middle of June and have increased slightly since. Note that the last couple weeks shown are very likely incorrect due to the time it takes to process death certificates and record cause(s) of death. What’s interesting to note here is that number of excess deaths each week is roughly in line with, but generally greater than, the weekly totals for deaths attributed to COVID-19. It’s not clear why this would be and I cannot imagine it could possibly be the result of suicide rates going up by over 50%. If this were the case, I would hope the CDC would be providing some data for that. However, the CDC is primarily concerned with diseases and the deaths caused by those diseases.
Thus, if you believe the death toll of COVID-19 is greatly exaggerated, you need to somehow explain how more than 200,000 extra people have died this year. To understand this in terms of other causes of death, it could be explained by a 200% increase in deaths from other respiratory diseases, a roughly 50% increase in deaths from heart disease or cancer, or a 1000% (10x) increase in the number of suicide deaths. It is simply extremely hard to explain how 200,000 deaths above normal over a six month period could possibly be explained by an increase in any particular cause. In that time frame, the TOTAL death rate has increased by over 20%. It’s hard to imagine a 20% increase in one cause of death, nonetheless in all causes of death.
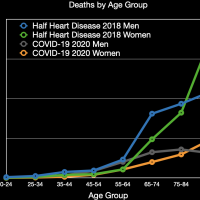
Once it’s clear that something is causing these extra deaths, people will then often say that it’s “just” old and/or sick people that are dying and that these people were going to die soon anyway. Looking at the data, the average age of a person dying from COVID-19 is around 73 years old for men and 79 years old for women, which makes it look like it’s just killing off the old people. Note that there is not data for COVID-19 deaths for each age, just age ranges. I took the middle of the range to determine the numbers above. I also calculated deaths from other diseases in this way and doing so shows that the group-age average is generally a couple of years older than the true average. For example, for heart diseases, the grouped averages are 77 and 83 for men and women, respectively, while the true averages are 74 and 81. The data also shows that the average number of comorbidities listed when COVID-19 was the primary cause is 2.6. However, it’s good to try to get some points of reference for these numbers. Thus, I looked at deaths from all respiratory illnesses, and pneumonia in particular, all cancer deaths, all deaths from heart disease, and all deaths from firearms to determine the average age of death and comorbidities for these causes.
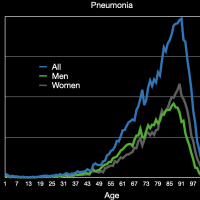
Let’s first look at pneumonia deaths as that disease is very similar to COVID-19. The average age of a person dying from pneumonia in 2018 was 79 years old–77.1 for men and 80.9 for women. Thus COVID-19 is killing slightly younger people than pneumonia does. For pneumonia, the average number of comorbidities listed is 1.8. It’s not really clear why this is significantly lower than for COVID-19, especially considering the value for all respiratory diseases provided below.
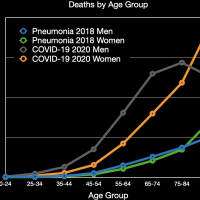
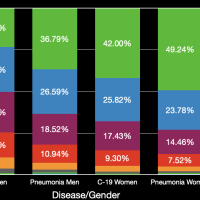
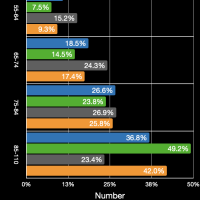
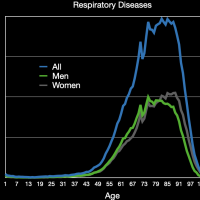
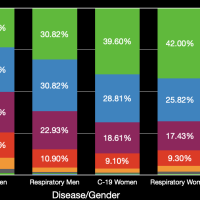
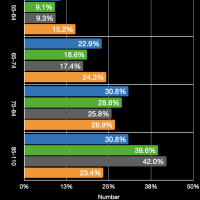
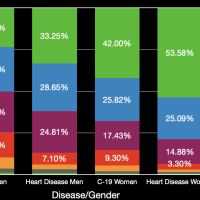
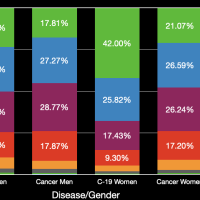
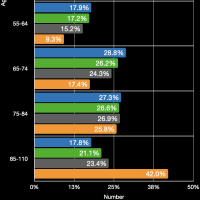
The images in the gallery (click to enlarge) above show how the ages breakdown for pneumonia and COVID-19 deaths for men and women. The first chart shows the age distribution of pneumonia deaths for men, women, and both in 2018. The peak for women occurs at 91 years old, for men at 88 years old, and for both combined at 91 years old. The second chart shows the number of deaths in the age groups the CDC tabulates for COVID-19 for each category. Note that these are pneumonia deaths for all of 2018 and COVID-19 deaths for about six months. Clearly the death rate for COVID-19 is much higher than that for pneumonia. The ages for pneumonia deaths also clearly skew higher, particularly for men. My first thought when I saw the curve for COVID-19 deaths for men was that the drop was simply the result that the population of men over 84 years old was much less than that from 75 to 84 years old. However, that drop is not present for pneumonia deaths. The next chart shows the percentage of deaths in each age group and in each category. This makes it very clear that COVID-19 is killing people quite a bit younger than pneumonia. The age difference is especially pronounced in men. The final chart shows the same data spread out so the percentages for the younger age groups can be seen. Even in the younger age groups, although the percentages are much smaller overall, it is clear that COVID-19 is killing people, both at a higher total number and higher percentages, younger than pneumonia typically does.
The average age of a person dying from any respiratory disease in 2018 was 77.1 years old–75.9 for men and 78.3 for women. Again, this is older than for COVID-19 deaths and these ages are a couple of years greater if we find the average from grouped ages. For all respiratory diseases, the number of comorbidities listed (i.e. in addition to the main cause of death) is 2.5 which is very similar to that of COVID-19. In general, it appears that respiratory disease deaths typically have more comorbidities listed than for deaths from other diseases. I suspect this is because deaths from a respiratory disease often involved multiple respiratory issues. This is why it is so surprising to me that the comorbidities for pneumonia are so low since pneumonia is frequently what kills people with immune diseases.
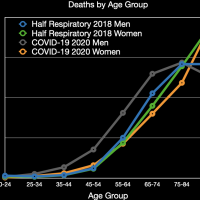
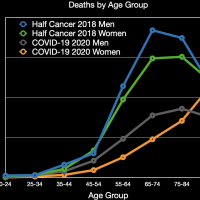
The images in the gallery (click to enlarge) above show how the ages breakdown for respiratory diseases and COVID-19 deaths for men and women. The first chart shows the age distribution of respiratory disease deaths for men, women, and both in 2018. The age range when the majority of people die from respiratory disease is large, between 75 and 90. The second chart shows the number of deaths in the age groups the CDC tabulates for COVID-19 for each category. Note that these are half the respiratory disease deaths for all of 2018 and COVID-19 deaths for about six months. The death rate for COVID-19 so far is fairly close to the death rate of women from all respiratory diseases in 2018. It appears that COVID-19 is much deadlier for younger men than all other respiratory diseases combined. The next chart shows the percentage of deaths in each age group and in each category. This makes it very clear that COVID-19 is killing people quite a bit younger than people dying from all respiratory diseases in 2018; this is especially true for men. The final chart shows the same data spread out so the percentages for the younger age groups can be seen. Even in the younger age groups, although the percentages are much smaller overall, it is clear that COVID-19 is killing people, both at a higher total number and higher percentages, younger than other respiratory diseases typically do. (The labels are incorrect.)
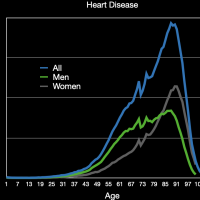
Turning our attention to heart disease we can clearly see that it is much more deadly to men at a younger age than it is to women. The average age of death from heart disease for men is 74 years old, and for women it is 81 years old. Note that both of these are older than the average age of a COVID-19 death. In fact, if you calculate the average for heart disease as I am forced to do for COVID-19, you get 77 years old for men and 83 years old for women. The average number of comorbidities for heart disease deaths is 2.3.
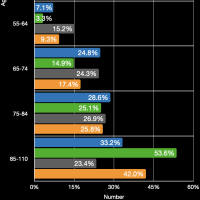
The images in the gallery (click to enlarge) above show how the ages breakdown for heart diseases and COVID-19 deaths for men and women. The first chart shows the age distribution of respiratory disease deaths for men, women, and both in 2018. Again we can see the clear difference in the ages when heart diseases kill men and women. The second chart shows the deaths grouped by ages so we can better compare with the COVID-19 data. Note that these are half the heart disease deaths for all of 2018 and COVID-19 deaths for about six months. For people (men and women) younger than 65 years old all heart diseases and COVID-19 kill at about the same rate. As a percentage of the total deaths, heart disease clearly kills people that are much older than those dying from COVID-19. For example, 25% of COVID-19 deaths for men have occurred for men 54 years old and younger. About half this percentage, 12.5%, of men dying from heart disease are younger than 55 years old. The data for women is again much different although relatively very similar. About 12.5% of women dying from COVID-19 are younger than 54 years old. Again, the percentage of women dying from heart disease who are under 55 years old is about half this. The bar chart breaks things out for each age group so the percentages for the younger ages are discernible.
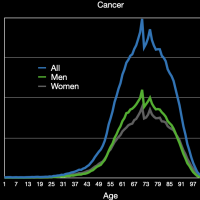
Cancer of course kills younger people, and we see that the average age for both men and women dying of cancer is about 71 years old and that is roughly the age at which most deaths occur. The number of comorbidities is 2.0 and, not surprisingly, less than for respiratory diseases.